 |
| Future world traveler |
Traveler's health includes
much more than infectious disease. More travelers die from cardiovascular
disease, motor vehicle accidents, and drowning than die from infectious
diseases. The most common infectious disease of travelers is traveler's diarrhea, which is usually self-limiting, but can be serious and can put a
vacationer out of commission for a substantial portion of a long-awaited trip.
Last month Mogens Jensenius and colleagues published a study of potentially life-threatening tropical diseases in travelers. Between June 1996 and August 2011 82,825
illnesses in travelers were reported to GeoSentinel. Of those,
3,666 (4.4%) had potentially life-threatening diseases. Falciparum malaria was by far the most frequently
reported potentially life-threatening disease.
I can't adequately address all of the aspects of traveler's
health here. I've included some resources below. Please note that immunization
recommendations and requirements for travel change, so I strongly recommend
consulting a travel medicine specialist at
least one month before your planned departure date.
There are three categories of travel immunizations: routine,
recommended, and required.
Routine immunizations
Outbreaks of diseases that have been eliminated from the U.S. continue to occur throughout the world, including outbreaks
of vaccine-preventable disease in wealthy countries:
All travelers should be up to date on all routine immunizations. Depending on age and destination, some travelers may require
booster doses.
Influenza
Unlike temperate
climates, there is no "flu season" in the tropics. Influenza is
transmitted year round, so travelers to tropical climates should receive an annual flu vaccine
at least two weeks prior to travel.
Measles, mumps, and
rubella
In 1989 the CDC's Advisory Committee on Immunization
Practices changed its recommendations from a single dose of measles, mumps, and rubella vaccine (MMR) to two doses. Adults who have received one dose
of MMR should receive a second dose. This recommendation includes
travelers to Europe. Nearly half of the measles cases imported into the U.S. in
2011 came from Europe.
Inactivated poliovirus
vaccine
Although wild poliovirus transmission has been interrupted
in all but three countries (Afghanistan, Nigeria, and Pakistan), a risk of
poliovirus infection to travelers exists in countries in which
- Oral poliovirus vaccine (OPV) is used
- Vaccine-associated paralytic polio (VAPP)
- Vaccine-derived polioviruses are circulating (cVDPV)
- Areas with inadequate immunization coverage
Recommended immunizations
Vaccines recommendations depend on the epidemiology of the
disease in the destination country and the age and health status of the
traveler. Recommended vaccines include hepatitis A, hepatitis B,
Japanese encephalitis, meningococcal,
pneumococcal,
typhoid,
varicella (chickenpox), and yellow fever
vaccines.
Notice that several of these vaccines are included
in the current ACIP childhood immunization schedules and may be
required for school admission. I'm only going to discuss the more "exotic"
diseases here.
Meningococcal vaccine
Meningococcus (Neisseria
meningitidis) is transmitted by respiratory droplets. As the name suggests,
meningococcus can cause bacterial meningitis (headache, photophobia,
stiff neck, confusion, and permanent neurological damage). Meningococcemia
(meningococcus in the blood) causes petechial rash, shock,
loss of fingers and limbs, and can be rapidly fatal.
Risk factors
for transmission include crowding, poverty, and smoking. Some people can carry
meningococcus without developing meningococcal disease (asymptomatic nasopharyngeal
carriage). Outbreaks usually occur in settings in which people live in close
contact with each other. In this country, those settings include college dormitories and military barracks.
Major meningococcal epidemics occur every 5 to 10 years in
the African Meningitis Belt. Epidemics occur during hot, dry, dusty seasons and
end at the beginning of the rainy season. I worked in Ethiopia during a
meningococcal epidemic. During the first three months of the epidemic we had no
vaccine and could only educate people about the symptoms of meningitis and
treat those who came to the health center.
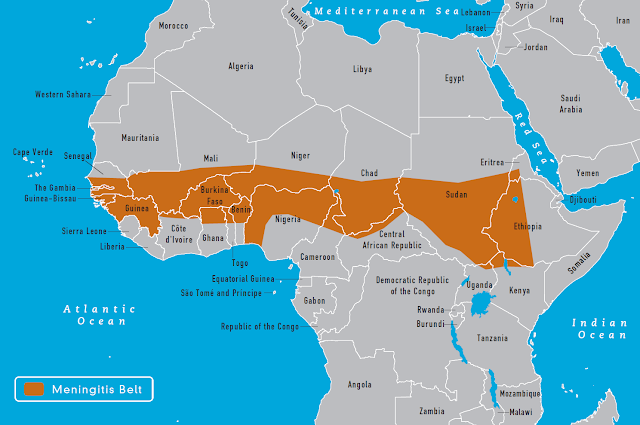 |
| CDC, 2012 |
Typhoid fever is caused by the bacteria, Salmonella enterica, subspecies Typhi.
Typhoid is transmitted by the fecal-oral route in areas with substandard
sanitation. There are several Salmonella
species that cause symptoms that are clinically indistinguishable from typhoid.
Symptoms include fever, relative bradycardia, abdominal pain, constipation
and/or diarrhea, headache, and mental status changes. Typhoid can be fatal if
not treated and resistance to antibiotics is becoming more common.
There are two typhoid vaccines licensed in the U.S.: Vivotif®,
a live attenuated oral typhoid vaccine and Typhim Vi®, an injectable
polysaccharide vaccine. Neither of these vaccines prevent non-typhoidal
Salmonella infections.
Japanese encephalitis
Like dengue, West Nile virus, and yellow fever, Japanese
encephalitis (JE) is caused by a flavivirus (flavi- "yellow") and is transmitted by mosquitoes. Most
infections are asymptomatic. About 1% of people infected with the Japanese
encephalitis virus will develop encephalitis. Symptoms include fever, headache,
lethargy, movement disorders, mental status changes, seizures, and focal
neurological deficits. Case fatality is around 20 to 30% and 30 to 50% of
survivors will be left with residual neurological deficits.
Most travelers to endemic countries are not at risk. The
risk is low in urban areas. Travelers who have long stays in or frequent
visits to rural/farming areas may be at risk. The JE vaccine available in the
U.S. is licensed for people 17 years of age and older. The vaccine is given in
two doses 28 days apart; the second dose must be given at least 1 week before
arriving in an endemic area. There is no JE vaccine available in the U.S. for
children 16 years of age and younger.
 |
| CDC, 2012 |
Yellow fever is endemic in parts of Africa and South
America. It was introduced to the United States via the slave trade and caused
major epidemics on the Eastern Seaboard and Mississippi Valley. Mosquito
control eliminated the disease from the U.S. The last major epidemic was in New
Orleans in 1905. Yellow fever is maintained in the wild in monkeys.
Most yellow fever virus infections are self-limiting.
Symptoms include fever, headache, and myalgias (muscle pain). Most people
recover without sequelae and immunity after infection is life-long. A minority
of people infected with the virus will appear to recover (period of remission)
and then develop serious illness (period of intoxication). The disease is
called yellow fever because it causes liver failure and jaundice. Twenty to
fifty percent of people who develop liver failure from yellow fever will die.
 |
| CDC, 2012 |
Required vaccines
When my family and I moved to Iran in 1978 there were three
vaccines required for international travel: cholera, smallpox, and yellow
fever. By the time I traveled to Africa for the first time ten years later,
there were two vaccines required for international travel: cholera and yellow
fever. Now there is only one vaccine required for international travel: yellow
fever.
Yellow fever vaccine must be given by a provider with an official uniform stamp who will issue a International
Certificate of Vaccination or Prophylaxis (ICVP) to the recipient. This
certificate is required for entry to Angola, Benin, Burkina Faso, Burundi,
Cameroon, Central African Republic, Republic of the Congo, Côte d’Ivoire,
Democratic Republic of Congo, French Guiana, Gabon, Ghana, Guinea-Bissau,
Liberia, Mali, Niger, Rwanda, São Tomé and Príncipe, Sierra Leone, and Togo.
Other countries may require yellow fever immunization for
people arriving from yellow fever-endemic countries.
Travel resources
Centers for Disease Control and Prevention (CDC): Traveler's Health
U.S. Department of State: International Travel
- General precautions
- Mode of travel: health considerations
- Other travel health risks
- Specific infectious diseases involving potential health risks for travellers
- Vaccines
- CDC: Travel Clinics
Alexander, J. P., Ehresmann, K., Seward, J., Wax, G.,
Harriman, K., Fuller, S. et al. (2009). Transmission of imported
vaccine-derived poliovirus in an undervaccinated community in Minnesota.
Journal of Infectious Diseases, 199(3), 391-397. http://jid.oxfordjournals.org/content/199/3/391.full.
Apicella, M. A. (2010). Neisseria meningitidis. In G. L. Mandell,
J. E. Bennett, & R. Dolin (Eds.) Mandell, Douglas, and Bennett's principles
and practice of infectious diseases, (7th Ed.). Elsevier [Electronic version].
Centers for Disease Control and Prevention. (1994). Typhoid
immunization recommendations of the Advisory Committee on Immunization
Practices (ACIP). Morbidity and Mortality
Weekly Report, 43(14), 1-7. http://www.cdc.gov/mmwr/preview/mmwrhtml/00035643.htm.
Centers for Disease Control and Prevention. (1998). Measles,
mumps, and rubella – vaccine use and strategies for elimination of measles,
rubella, and congenital rubella syndrome and control of mumps: recommendations
of the Advisory Committee on Immunization Practices (ACIP). Morbidity and Mortality Weekly Report,
47(8), 1-57. http://www.cdc.gov/mmwr/preview/mmwrhtml/00053391.htm
Centers for Disease Control and Prevention. (2006). Imported
vaccine-associated paralytic poliomyelitis – United States, 2005. Morbidity and Mortality Weekly Report, 55(4),
97-99. http://www.cdc.gov/mmwr/preview/mmwrhtml/mm5504a2.htm.
Centers for Disease Control and Prevention. (2010). Japanese
encephalitis vaccines. Recommendations of the Advisory Committee on
Immunization Practices (ACIP). Morbidity
and Mortality Weekly Report, 59(1), 1-27. http://www.cdc.gov/mmwr/preview/mmwrhtml/rr5901a1.htm.
Centers for Disease Control and Prevention. (2012). CDC health information for international
travel 2012. New York: Oxford University Press. [Electronic version].
http://wwwnc.cdc.gov/travel/page/yellowbook-2012-home.htm.
Centers for Disease Control and Prevention. (2012). Measles
– United States, 2011. Morbidity and
Mortality Weekly Report, 61(15), 253-257. http://www.cdc.gov/mmwr/preview/mmwrhtml/mm6115a1.htm.
Jensenius, M., Han. P. V., Schlagenhauf, P., Schwartz, E.,
Parola, P., Castelli, F. et al. (2013). Acute and potentially life-threatening
tropical diseases in western travelers – a GeoSentinal multicenter study,
1996-2011. American Journal of Tropical
Medicine and Hygiene, 88(2), 397-404. http://www.ajtmh.org/content/88/2/397.full.
Jong, E. C. (2008). Immunizations for travelers. In E. C.
Jong & C. Sanford (Eds.) Travel and
tropical medicine manual. (4th Ed.). Elsevier. [Electronic version].
Steffen, R. & Grieve, S. (2013). Epidemiology: morbidity
and mortality in travelers. In J. S. Keystone, D. O. Freedman, P. E. Kozarsky,
B. A. Connor, & H. D. Nothdurft (Eds.) Travel
medicine (3rd Ed.). Elsevier. [Electronic version].
Thielman, N. M., Crump, J. A., & Guerrant, R. L. (2010).
Enteric fever and other causes of abdominal symptoms with fever. In G. L.
Mandell, J. E. Bennett, & R. Dolin (Eds.) Mandell, Douglas, and Bennett's principles and practice of infectious
diseases, (7th Ed.). Elsevier [Electronic version].
Vaughn, D. W., Barrett, A., Solomon, T. (2010). Flaviviruses
(yellow fever, dengue, dengue hemorrhagic fever, Japanese encephalitis, West
Nile encephalitis, St. Louis encephalitis, tick-borne encephalitis). In G. L.
Mandell, J. E. Bennett, & R. Dolin (Eds.) Mandell, Douglas, and Bennett's principles and practice of infectious
diseases, (7th Ed.). Elsevier [Electronic version].

No comments:
Post a Comment